“Beam me up, Scotty”
-Capt. Kirk of Star Trek, the Original, 1960’s
The Massachusetts Public Health Council has approved the construction of a proton beam therapy (PBT) center in Boston by Dana-Farber Cancer Institute for an estimated cost of $50 million. It is the fourth to be approved in Massachusetts; one operating now and a second one to be reopened in June 2027 by Mass General Brigham. A fourth will be built in Central Mass by UMass Memorial Health Care. There are 48 operating PBT units in the U.S. There are two in the U.K.; one in London and one in Manchester.(1)
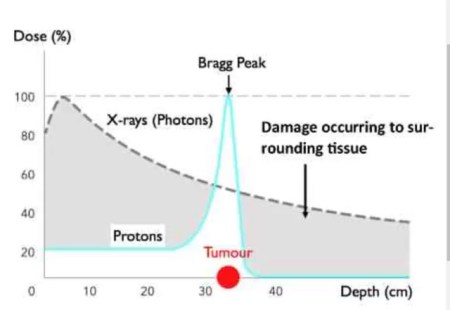
Proton beam therapy is a new technology to cure or shrink certain cancers. It is a high energy invisible beam that travels through normal tissue with little or no damage to deliver its cellular killing energy directly to the deep tumor. The energy delivery is at Bragg Peak, 12 to 14 inches deep in the body. Calibrating the beam energy can vary the specific target distance.
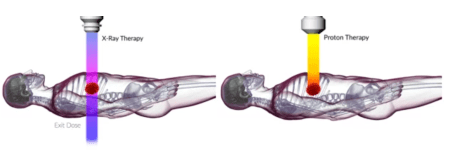
Unlike X-rays which can pass through the tumor and damage other tissue on the other side of the tumor, the proton beam expends almost all of its energy at the tumor site. Their is less tissue damage beyond the tumor. This type of pinpoint radiation avoids most of the side-effects caused by more traditional x-ray (photon) radiation therapy.
Obviously this is a great advantage when treating deep tumors in the brain, prostate, liver, breast, and pancreas; or tumors of the eye, head and neck. PBT has been available in the U.S. since 2004 and its use is increasing. Improved outcome results (“curative” or “growth controlling”) from PBT have been variable depending on type of cancer, body site, and facility.
The expectation has been that PBT will have better outcomes than traditional radiation for those tumors with complex anatomy, sensitive surrounding tissues, or in children. , but improved outcomes over X-ray therapy has been successfully achieved in only certain tumors in specific body sites. Studies of eligibility criteria and PBT outcomes continue.
Senator Kennedy’s resorting to PBT at MGH in 2009 for treatment of his brain tumor (covered by Medicare) which did not obtain any real benefit spurred interest in developing clear criteria for use of this expensive resource. Dr. Fergus Macbeth, director of U.K.’s Center for Clinical Practice and a specialist in radiation therapy for cancer, said in 2009 that if Kennedy had been a patient in Britain’s National Health Service “he wouldn’t get proton beam therapy. And there’s absolutely no evidence [in 2009] that proton beam therapy provides any additional benefit. It’s not a wise use of your resources.”
A 2025 comparison study of 1200 breast cancer patients receiving either traditional X-ray radiation or proton beam therapy in 32 U.S. Centers showed that both groups had similarly improved outcomes with only a slightly larger patient satisfaction rating with proton therapy. (The study was not blinded because the beam machine looks so unique , so PBT patients knew they were getting the “brand new” treatment.) Side effects were minimal in both groups.
Because of the current lack of compelling outcome benefit data, health insurance coverage for PBT can vary by state, insurance company, or agency. The base cost of PBT in the United States typically ranges from $30,000 to $180,000 or more. This figure encompasses the PBT itself and diagnostic MRIs and CT scans, pre-treatment planning, ancillary medical services, and oncology consultations. The actual PBT session typically costs between $1,000 and $3,000. The total number of sessions varies depending on the cancer type and stage, but a typical course of treatment might involve 20 to 40 sessions.
Since PBT currently has select, but limited proven benefits, eligibility criteria, and variable insurance coverage, the optimal use of PBT for cancer treatment is best informed by a cost-benefit analysis of the patient’s well-being expectations by the patient/family and the radiation oncology team in each case.